
Team
members from The Family Van stand in front of the mobile clinic. The
van focuses its efforts in Roxbury, Dorchester and East Boston with a
rotating weekly schedule.
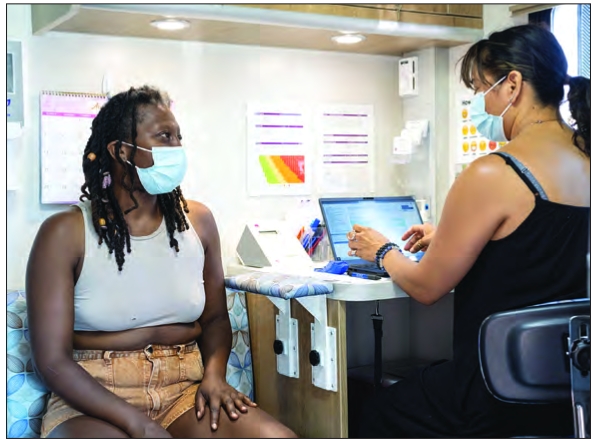
A Healthy Roads community health worker meets with a patient.
Free program offers personlized support with focus on coping strategies and mental well-being
For community health workers and staff at The Family Van, a Boston-area mobile health clinic, there’s magic in connecting with community members to offer and something special in the simple questions like, “How are you?”
Through its program Healthy Roads, staff at The Family Van, which is associated with Harvard Medical School, is trying to bring that magic beyond just physical health and into mental health care as well.
“We always talk about wellness, because we want to see somebody well from the head to the toe. We think about the total health care of the individual that’s in front of us,” said Rainelle Walker-White, associate director health equity programs with The Family Van.
Launched in 2021, the Healthy Roads program uses Problem Management Plus, a curriculum developed by the World Health Organization, to teach coping strategies and problem-solving skills to reduce symptoms of anxiety and depression.
The program was featured at Boston Medical Center’s Sept. 12 health equity summit, EQTY 2024, as an innovative approach to providing care.
Through the program, six community health workers and more than 87 volunteers, medical students and interns at The Family Van offer clients five free sessions to learn skills to cope with and work through stressors, like breathing techniques, how to access social supports and how a client can move into action to manage their care.
According to its 2023 impact report, the group reported benefits like improved social connection, increased physical activity, better sleep and increased confidence and hope.
In developing it, Piper Derenoncourt, assistant
director of mental health equity programs, said The Family Van aimed to
really center the voices and needs of the communities they serve.
Listening to the community
For
example, the WorId Health Organization’s original curriculum outlines
90-minute sessions, but in some of the initial conversations with
communities the organization held to structure the program, Derenoncourt
said they heard suggestions like 30 minutes every other week was more
functional, and that they should be run by people from the community
rather than social workers.
“We
leaned into that, and we do lean into that,” she said. “There are times
where it might be 15 minutes that someone has, and there are sessions
that might run a little longer.”
That
means that the work addresses some general stressors — like
dissatisfaction at work or relationship issues or facing unemployment —
but also others like struggling with language barriers or facing the
challenges of the U.S. immigration system.
The Healthy Roads effort aims to change what mental health care and access to that care looks like.
“We
must reimagine mental health care and expand our thinking about who,
how and where care can be delivered,” said Mollie Williams, executive
director of The Family Van at a presentation at BMC’s health equity
summit. “That’s what we’re working towards, a city, really not just a
city, a world, where everyone can thrive.”
A
big part of that reimagining is bringing care beyond specialists like
psychologists and psychiatrists to connect more people with the basics
that can help them in their day-to-day lives.
“Not
everyone needs [to talk to a psychiatrist or a psychologist],”
Derenoncourt said. “How do we build out the community-level support
where we’re not diagnosing, we’re focused on promoting well-being and
helping people just talk about their mental well-being or connecting
with each other.”
Meeting clients where they are
Staff
at The Family Van said they think that the community health workers who
help clients through the Healthy Roads program may be more
approachable.
They don’t wear lab coats and don’t offer session through a sterile hospital setting.
Instead,
they often meet clients in the community, at a Dunkin’ or a library or
on a park bench during the gap before a parent has to pick up their
child. Clients can also opt to do their sessions on Zoom.
“For
a community health worker to work with somebody around their mental
health, I think that connection and that engagement is so much more
empathetic, but at the same time, it’s comforting.” Walker-White said.
Derenoncourt
said The Family Van has received feedback from clients who are also
seeking services from a therapist revealing that they can talk more
openly with their community health worker than with the mental health
specialist.
“We get so
caught up in metrics, how we can measure things and best practices and
evidence-based, that sometimes we lose the magic that really is within
healing, and that’s connecting with people,” Derenoncourt said.
T hat on-the-ground connection can help some
clients who might struggle with the stigma around mental health care to
be willing to access the services through the Healthy Roads program.
“The
biggest thing that we’ve learned is that we don’t really have to
promote it as mental health or well-being; that will automatically
create barriers for people,” she said. “So, how are we talking about it
in a way that people can relate and really see themselves?”
Instead,
they often let it be a natural offshoot of conversations with clients
about how they’re doing and what needs aren’t being met, said Dina
Martinez, a community health worker with the van.
“We
see [other challenges with well-being] as a way of communicating,”
Martinez said. “‘I am under stress because I’m not sleeping,’ ‘I am
under stress or depressed because I’m not eating well.’ There’s that
listening piece. The client always communicates, ‘I’m not well’ in many,
many forms.”
Reimagining
care isn’t new for the group, which has been going out to provide care
directly in communities for decades. The mobile clinic — which regularly
provides free health screenings, education and community referrals —
was first launched in 1992.
Small actions, big impact
In
2023, the group reported over 1,700 visits to the van and 3,000
preventive screenings to community members, according to its annual
impact report.
Those
screenings were for physical health issues, including things like blood
pressure, blood glucose, obesity and pregnancy, but also mental health
topics like anxiety and depression.
And
that impact overwhelmingly affected communities of color. The van
focuses its efforts in Roxbury, Dorchester and East Boston with a
rotating weekly schedule. The report indicated that 94% of the clients
they worked with were people of color and over 50% primarily spoke a
language other than English.
Helping
to bridge language barriers can be an important step to reducing
stressors. Martinez said one client she worked with at The Family Van
didn’t speak English, so as part of helping him, they found him online
language classes. Partway through the five sessions, he came back and
asked to start doing the Healthy Roads meetings in English.
“That,
to me, is a success, right?” Martinez said. “That the fact that he felt
so much better about himself, so much more confident about seeking work
and just communicating in life in the secondary language that he’s
learning, that is really good. It’s a successful story for him and for
us at the Van.”
Steps
like that — non-traditional ones that can bring new types of care to the
community — are some of the things staff at The Family Van point to as
actions that can address equity disparities more generally.
“I
believe that we can change these systems,” Williams said, during her
presentation at the EQTY summit. “I believe that we can work together to
ensure that people get the help they need and deserve so that everyone
can live full, healthy lives.”